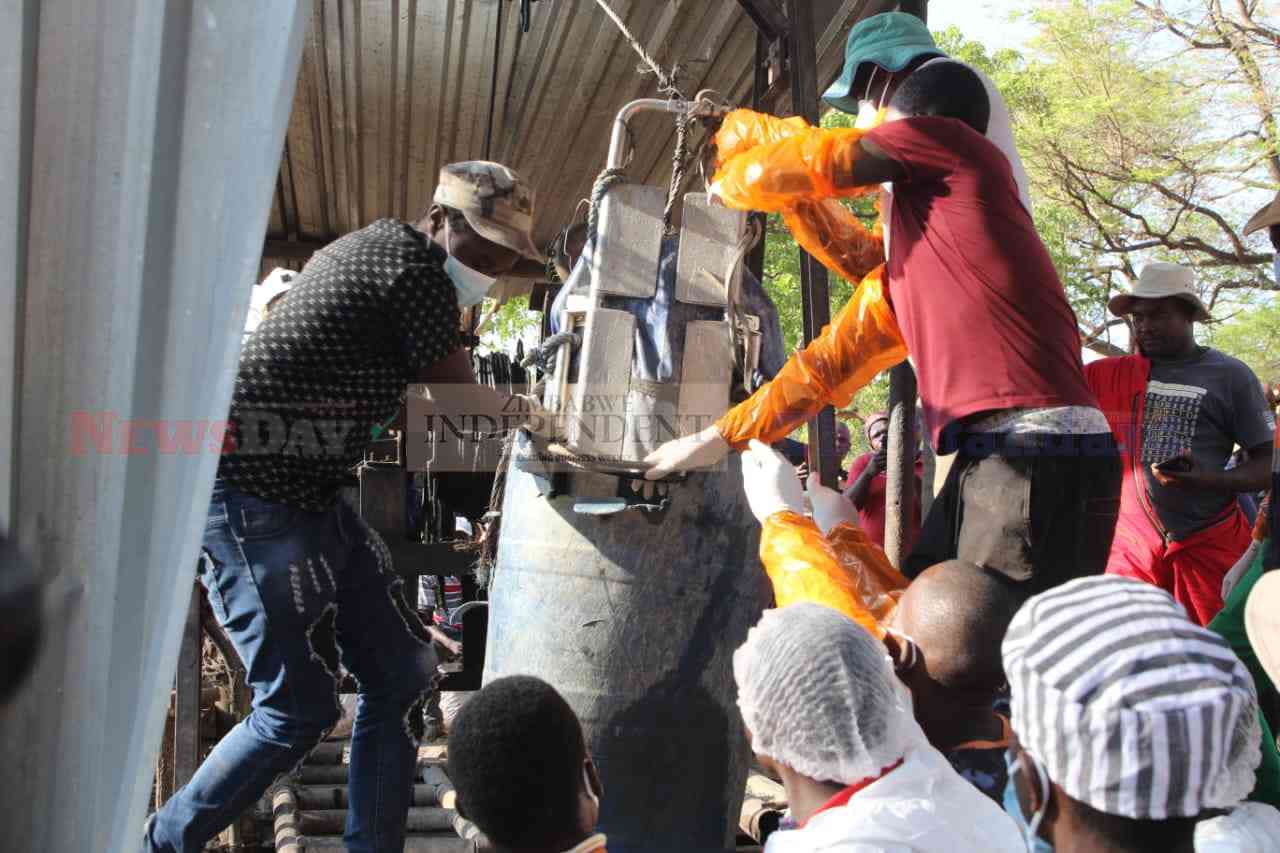Zanu PF bigwigs denied Uhuru freebies
Local News
By Problem Masau
| 11h ago

However, Zanu PF director for information Farai Marapira said there might have been a “glitch” for the bigwigs not to get fuel and accommodation.
.
Videos
Pamela Marwisa In Conversation With Trevor
By The NewsDay
Feb. 28, 2024
By The NewsDay
Feb. 28, 2024
By The NewsDay
Dec. 5, 2023
Old Mutual launches funeral services in Masvingo
Sponsored Content
Vintage travel and tours reveals its successes
Sponsored Content
EcoCash extends payroll services to security companies
Sponsored Content
Demand for milk seen softening
Morgan & Co estimated a FY24 price target of US$0,0943 that is largely driven by an enterprise value to its earnings before interest, taxes, depreciation and amortisation valuation.
By Mthandazo Nyoni
Apr. 18, 2024
Govt sets target for winter wheat production
By Priviledge Gumbodete
Apr. 17, 2024
El Niño drives Zimbabwean millers to seek Brazilian corn
By Bloomberg News
Apr. 16, 2024
Govt to clamp down on cotton side marketers
By Blessed Ndlovu
Apr. 11, 2024
High rabbit pellets prices choke Zimbabwe farmers
By Mthandazo Nyoni
Apr. 5, 2024
Govt sets target for winter wheat cropping
By Harriet Chikandiwa
Mar. 30, 2024
Smart farming to fight El Nino
By Nhau Mangirazi
Mar. 30, 2024
CIMMYT develops multiple stress tolerant maize varieties
By Mthandazo Nyoni
Mar. 28, 2024
No room for politicking in food distribution
By Newsday
Apr. 17, 2024
Bullying tactics will not work
By Newsday
Apr. 16, 2024
ZiG: Guard against political interference
By Newsday
Apr. 15, 2024
Availability will stabilise sugar prices
By Newsday
Apr. 13, 2024
Moral suasion key for currency survival
By Newsday
Apr. 12, 2024
Shot in the arm for the Deeds Registry
By Business Reporter
Apr. 18, 2024
Mind your pricing regime, HAZ warns operators
By Freeman Makopa
Apr. 17, 2024
Old Mutual thumbs up new MPS measures
By Melody Chikono
Apr. 17, 2024
Access to credit by women improves
By Mthandazo Nyoni
Apr. 17, 2024
It won’t be business as usual, RBZ boss tells staff
By Mthandazo Nyoni
Apr. 17, 2024
Premier seeks US$3,74 million for Zulu project
By Mthandazo Nyoni
Apr. 16, 2024
.
Sport
NewsDay cartoon 28 November, 2023 edition
NewsDay cartoon 28 November, 2023 edition
By The Watcher
Nov. 28, 2023
Govt urges unity among lithium miners
Currently there are around eight different lithium exploration and mining projects at different development stages.
By Mthandazo Nyoni
Jun. 1, 2023
Over 130 civilians killed by DR Congo rebels - UN
By BBC News
Dec. 8, 2022
Opaque Chinese deals: Mthuli taken to task
By admin
Aug. 29, 2022
Power outages, raw material shortages hit ART operations
By The NewsDay
Aug. 17, 2022
We’re unstoppable: CCC
By The NewsDay
Aug. 16, 2022
Umzingwane, Matobo main road ‘forgotten’
Matobo ward 15 councillor Dickson Moyo said the Old Gwanda road, which is major road passing through Umzingane and Matobo, had been neglected for more than five years.
By The NewsDay
Jul. 29, 2022
Diasporas must vote in Zim elections

The Zimbabwe Diaspora Vote Initiative closely followed the Russian elections, monitoring how the Russian government handled diaspora voting in that election.
By AMH Voices
Apr. 6, 2024
Lady Chevrons vie for World Cup place
By AUSTIN KARONGA
Apr. 14, 2024
Youth move in to get slice of construction industry cake
Chihota gave thumbs up to the parent association, ZBCA, for coming up with such an initiative.
By Staff Reporter
Apr. 14, 2024
Makarati boost for DeMbare
By Henry Mhara
Apr. 14, 2024
Scores arrested for booing Auxillia
By KUMBIRAI MAFUNDA and Everson Mushava
Apr. 14, 2024
Champions Ngezi Platinum snatch point from Bosso
By Munyaradzi Madzokere
Apr. 14, 2024
Govt fails to pay civil servants for blitz
By Miriam Mangwaya
Apr. 14, 2024
Farmers lose livestock to harmful mining practices
An affected farmer himself, Chief Masuku, called for stakeholder concerted interventions to ensure responsible mining activities to preserve the environment.
By Rex Mphisa
11h ago
Overflowing toilets a health time bomb
By JERSSIE MPOFU
Apr. 18, 2024
Women dominate vending in Bulawayo: Report
By Innocent Magondo
Apr. 18, 2024
NGO mobilises sanitary wear for women in prison, girls
By Patricia Sibanda
Apr. 18, 2024
De Souza banks on speed, agility.

Zimbabwe U20 rugby team head coach, Shaun De Souza is happy with the team’s preparations and looking forward to their tournament opener against Tunisia.
By AUSTIN KARONGA
1h ago